After the emotional journey that was my earlier post, I thought it was really important to have a more matter-of-fact run down of my rheumatology appointment today, as I learned a lot about self-advocacy and how to try and find that balance between presenting a considered suggestion, and telling the doctor how to do their job.

At 8am, I hobbled up the incredibly steep stairs to this new clinic that, despite having driven past for at least ten years, I’d never noticed before. (There was a ramp, but I’m still in the denial phase about my mobility, even though I’m still on the crutch).
The new patient checkin was nothing new, give them my medicare information, and sell my soul by not reading the terms and conditions before signing it away.
(who am I kidding, I’m a law student, I’m the kind of nerd who actually reads the T&C’s)
The thing that did surprise me was the efficiency. No sooner had the clock gone 8.15 and my doctor was popping out to call me through. He’d already had a read of my referral, and he went through the major points that my GP had listed, which were relatively minimal as she’s not a hypermobility or joint specialist. The thing that was new to me was that instead of directly asking me about and moving to treat just those symptoms listed, he then asked me what my concerns were, and he listened.
I told him about my informal diagnoses of hypermobility, and how when I had researched EDS based on a few off-hand queries from other doctors, reading peer-reviewed journal articles felt like reading my own medical history. I gave him the letters from the other members of my care team, the angels who despite my brain-fogged self only giving them 3 days notice, had written incredibly detailed reports showing how my joint laxity was causing chronic pain and recurrent injury. When he asked me about my symptoms, and I began reading from the file I had put together listing my symptoms, major medical events, and history of scans, he not only asked to read them himself, he also complimented me on being proactive about my health and asked me to email him copies.
Then came the moment that I’d been dreading, a diagnosis that I’d heard rumours was an “it’s all in your head” diagnosis – fibromyalgia. But I think he could see me panic, and he said to me – “I definitely agree that you seem a likely candidate for EDS, but you seem super knowledgable about it, so I don’t need to educate you on that, but this is something which I think could really help” – so I held my breath and waited, trying to put my anxiety on hold. And things started to make sense. He looked at the autonomic symptoms that I had been experiencing, and told me how they might be related. He asked me if I’d ever seen sleep graphed out in stages, and showed me an unaffected brain in comparison to a fibromyalgia one. I’ve never had a sleep study, but I’ve been tracking my sleep, for both quality and quantity (or lack thereof), on my Fitbit for ages, and when my doctor held it up next to his textbook photo, they were almost identical. We talked about how my nervous system was essentially on fire, and that was why my current pain medications weren’t working, and I’m so excited to be starting a new treatment plan, first tinkering with my current depression medication, and then once my acute hip injury recovers some more looking at a long term medication for pain management.
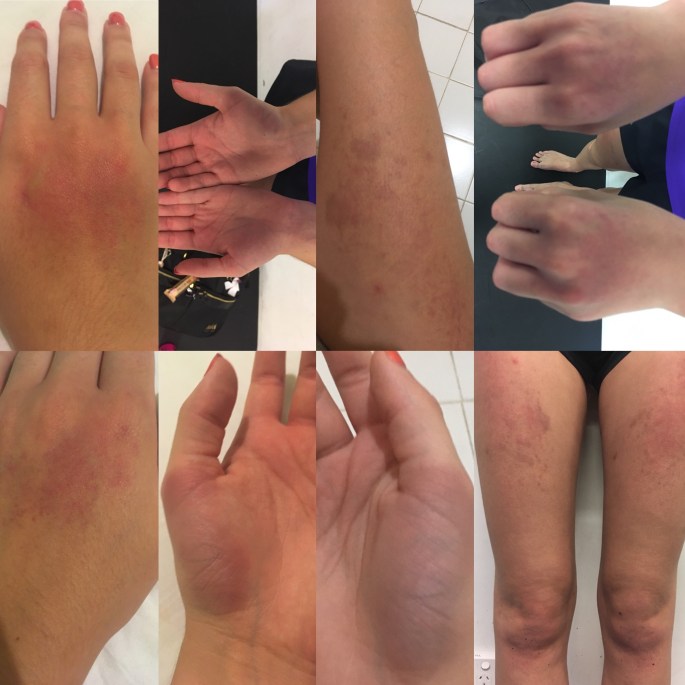
We then got to the part of the examination that I was hoping would come but still half-expecting wouldn’t happen, my assessment against the formal 2017 hEDS criteria. For ease, I’d brought along the checklist with me, but I was shocked to learn that my rheumatologist had multiple EDS patients, so he knew what to look and ask for without having to refer to it. The one scary part was when we were testing my mobility and I had to reach my hands to the floor, which is how I subluxed my hip, but I at least got my fingers flat on the ground before things started hurting and feeling unstable, which he said was sufficient considering I was injured. Also, I managed to shock him with the amount of bruising I’d had in the past (I’ll post photos below for the morbidly curious) and made me realise how genuinely stretchy my skin was. Like, I knew it was a bit stretchy, but not as out of the ordinary as it actually is. When I asked for something formal in writing with my diagnosis, as I’ve had doctors, particularly hospitals, doubt my dislocations in the past, he joked “if anyone doubts you’ve got EDS, just show them your skin”.
I’m also super grateful that he’s looking into a bulk-billed geneticist for me when I mentioned I couldn’t really afford to see too many more specialists, and also charged me the pensioner rate despite me not being an actual old person (but tbh I’ve met old ladies who are much healthier than me so …)
For the first time in a long time, I have hope, I have answers, and I’m actually looking forward to learning more about my health and taking a more active role in my treatment.
P.s. I know for EDS this isn’t too crazy, but these are the only cute ‘stretchy’ photos I’ve got
I can’t believe ever thought my skin was normal!
For anyone interested, these are the sleep graphs I mentioned:
- The blue graph maps “normal” sleep
- The green maps the typical sleep pattern for someone with fibromyalgia; showing little deep sleep (the restful kind), which is part of what contributes to the chronic fatigue
- The last two are examples of two nights within the last month or so from my Fitbit
I originally purchased my Fitbit Alta HR to track my heart rate while exercising, and to also keep an eye on what my sleep was doing because I knew it wasn’t all that great, but it looks like its going to be a valuable tool to see the effects of different treatment

As promised, the bruise photos are below:





One thought on “The Revolutionary Rheumatologist”